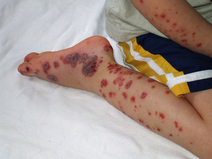
Idiopathic Thrombocytopaenic Purpura (ITP)
Epidemiology
Aetiology
Clinical Features
cf. HSP: no abdo pain, excessive bleeding (though rare. epistaxis 3% intracranial haemorrhage 1%)
Investigations
Bloods:
Others:
cf HSP: abnormal platelet count
Management
Source
Toronto Notes 2012
- •Most common cause of thrombocytopenia in childhood
- Peak age: 2-6 yrs, M=F
- Incidence 5 in 100,000 children per year
Aetiology
- Autoantibodies binding to platelet membranes --> Fc-receptor mediated splenic uptake --> destruction of platelets
- 50% present 1-3 wks after viral illness (URTI, chicken pox)
Clinical Features
- Sudden petechiae, purpura, epistaxis
- No lymphadenopathy, no hepatosplenomegaly (leukaemia, autoimmune, infection)
cf. HSP: no abdo pain, excessive bleeding (though rare. epistaxis 3% intracranial haemorrhage 1%)
Investigations
Bloods:
- FBC (thrombocytopenia with normal RBC, WBC)
Others:
- Bone marrow aspirate only if atypical presentation
cf HSP: abnormal platelet count
Management
- Spontaneous recovery in > 70% of cases within 3 months
- Treatment with IVIG, prednisone or IV anti-DIg (if Rh D+) if mucosal or internal bleeding, platelets <10, or at-risk of significant bleeding (surgery, dental procedure, concommitant vasculitis or coagulopathy)
- Life-threatening bleed: additional platelet transfusion± emergency splenectomy
- Chronic (>3-6 months): re-evaluate; treat if symptoms persist
- Supportive: avoid contact sports and ASA/NSAIDs
Source
Toronto Notes 2012