Abnormal Presentations and Multiple Pregnancies
Epidemiology
Normal = Occipitoanterior
Most frequent to least:
OP
Breech
Normal = Occipitoanterior
Most frequent to least:
- Occipitoposterior (OP) (10%)
- Breech (3%)
- Face (0.2%)
- Transverse
- Brow (0.07%)
OP
- Labour prolonged
- If 2nd stage >2h, need help (CS, forceps, ventouse)
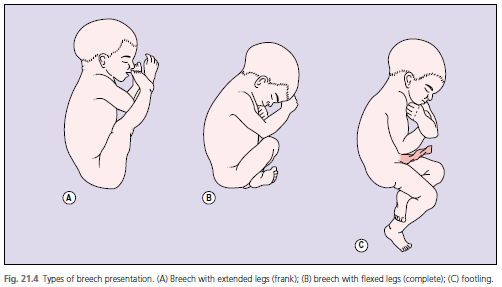
Breech
- Types: Frank (Toes to face), Complete (Cross legged), Footling (standing one 1 leg)
- No worries before 35/40
- External cephalic version by 37/40 (easier if complete/ footling)
- Rx: Elective CS
Face
Transverse/ Oblique/ Shoulder
Brow
Multiple pregnancy (1%)
Definition
Risk Factors
Issues
Management
Source
Llewellyn-Jones 9th Ed 2010
- Rarely dx before labour
- Facial oedema
- Rx: Forceps/ CS if needed
Transverse/ Oblique/ Shoulder
- May be associated with polyhyrdramnios, placenta previa, uterine malformation
- Rx: Exclude placenta previa --> ECV, admit to await labour/ CS (if late detection)
Brow
- Usually converted to cephalic presentation
- US to exclude foetal malformations (esp hydrocephaly)
- Rx: CS unless foetus dead
Multiple pregnancy (1%)
Definition
- Dizygotic (DZ) = 2 or more ova released and fertilised = own placenta, amnion+chorion
- Monozygotic (MZ) = 1 fertilised ovum divides early (inner cell mass stage) to form 2 identical embryos = 1 placenta + own sac (98%)
- Twins 1/90
- Triplets 1/90x90 = 8100
Risk Factors
- Age
- Multiparity
- Maternal FHx
- Ethnic (African>Caucasian>Asian)
- IVF
Issues
- MZ sharing same sac (2%) risk of cord entanglement
- MZ, 1 reduced supply of nutrients = IUGR, twin-twin transfusion = polyhydramnios, anaemia, oligohydramnios, polycythaemia, hypervolaemia, cardiac failure, death
- Usually smaller than singelton foetus
- Triplets 80% preterm = CS
- Main foetal risk (compared to singleton) is preterm birth (eg. cerebral palsy)
Management
- Fortnightly antenatal visits: check for anaemia, US for foetal growth (twin-twin transfusion)
- Inc folate, Fe
- Can NVD (if both cephalic or can ECV)/ CS (if breech, complications)
- Expedite delivery if bad blood flow
Source
Llewellyn-Jones 9th Ed 2010